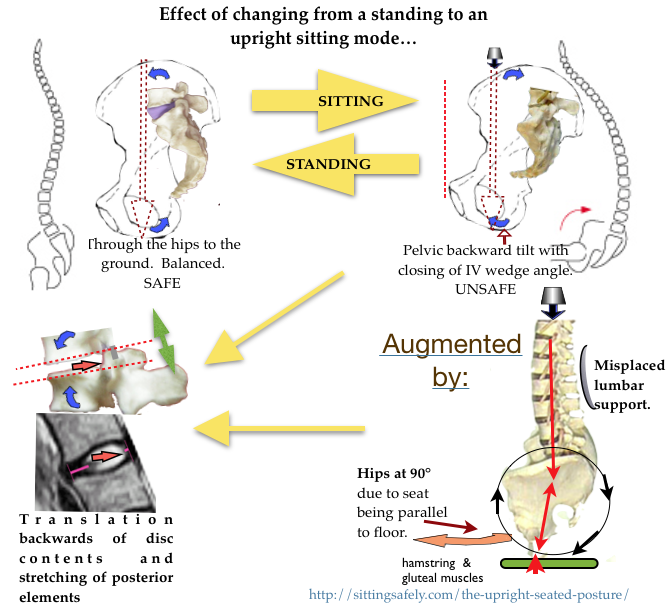
The bio-mechanical factors and their effects that may determine spinal pathology and lead to backache (Low Back Pain. LBP & further pathology) are discussed.
 The final common pathway …
The final common pathway …
to IV Disc pathology at the joints of the lumbar-sacral junction (L3/4, L4/5, L5/S1) is reduction of the L/S joint angle resulting in posterior movement of the intervertebral disc (IVD) contents and can be seen, on pMRI scan (Smith F 2006). This retropulsion of disc contents can progress to protrusion and extrusion (see ☛The intervertebral disc→). Also CTD→
1. Axial loading.
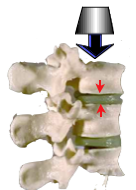 With the currently advocated upright sitting posture there is an increase of compression on the L3 disc is x2.5 above that when lying supine (Nachemson). This has been questioned by later work and determined by Wilke (Wilke1999) as 0.10 MPa for standing and sitting 0.55 MPa. With the currently advocated upright sitting posture there is an increase of spinal loading 500% above that of lying supine which is relevant to the 2T reclined mode. For more detail see ☛ Loading→
With the currently advocated upright sitting posture there is an increase of compression on the L3 disc is x2.5 above that when lying supine (Nachemson). This has been questioned by later work and determined by Wilke (Wilke1999) as 0.10 MPa for standing and sitting 0.55 MPa. With the currently advocated upright sitting posture there is an increase of spinal loading 500% above that of lying supine which is relevant to the 2T reclined mode. For more detail see ☛ Loading→
The intra-discal pressure is augmented In the flexed position, largely due to tension of the posterior ligaments, while the anterior portion of the annulus fibrosis (AF) undergoes compression In full flexion this can be as much as 100%. The pressure gradient increases anteriorly, tending to retropulsion of the nucleus pulposus (NP).
2. Axial compression + flexion.
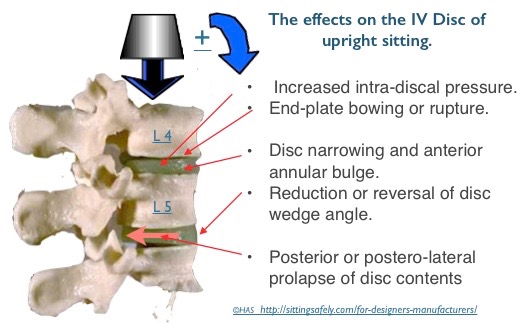 Disc prolapse occurred more frequently when the vertebral segments were wedged to simulate extreme forward bending of the spine (Adams and Hutton, 1982). In this position, the anterior portion of the annulus fibrosis undergoes compression while the posterior portion is under tensile stress. Over 40% of the cadaver discs tested by Adams and Hutton (1982) prolapsed when tested in this hyper flexed posture, and with an average of only 5,400 N of compression force applied. This finding shows that the disc is particularly susceptible to bending stresses. In a later study in which Adams and Hutton (1985) simulated repetitive loading of the disc, previously healthy discs failed at 3,800 N, again mostly through trabecular fractures of the vertebral bodies. Taken together, these studies show that the disc, especially the vertebral endplate, is susceptible to damage when loading is repetitive or when exposed to large compressive forces while in a severely flexed posture.
Disc prolapse occurred more frequently when the vertebral segments were wedged to simulate extreme forward bending of the spine (Adams and Hutton, 1982). In this position, the anterior portion of the annulus fibrosis undergoes compression while the posterior portion is under tensile stress. Over 40% of the cadaver discs tested by Adams and Hutton (1982) prolapsed when tested in this hyper flexed posture, and with an average of only 5,400 N of compression force applied. This finding shows that the disc is particularly susceptible to bending stresses. In a later study in which Adams and Hutton (1985) simulated repetitive loading of the disc, previously healthy discs failed at 3,800 N, again mostly through trabecular fractures of the vertebral bodies. Taken together, these studies show that the disc, especially the vertebral endplate, is susceptible to damage when loading is repetitive or when exposed to large compressive forces while in a severely flexed posture.
3. Backward pelvic tilt. An effect of upright sitting.
When sitting there is backward tilting (anat; forward rotation) of the pelvis, which reduces or reverses the protective wedge angle of the lower lumbar joints ☛(See Lumbar & spinal support→).
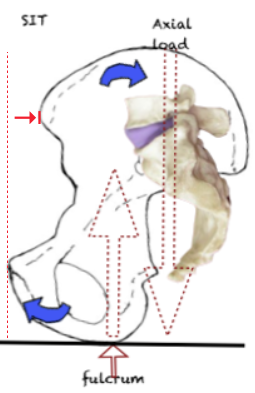 ←Flexion The axial loading force comes to lie posterior to the pivot point at the Ischial Tuberosities. A backward turning movement results in backward tilt in of the pelvis.
←Flexion The axial loading force comes to lie posterior to the pivot point at the Ischial Tuberosities. A backward turning movement results in backward tilt in of the pelvis.
- The backward pelvic tilt flattens the lumbar lordosis and reduces
 the protective wedge angle of the lower intervertebral discs. Resulting in Posterior translation of the disc contents (NP),, see below→
the protective wedge angle of the lower intervertebral discs. Resulting in Posterior translation of the disc contents (NP),, see below→
- The loss of low lumbar lordosis reduces or even reverses the protective wedge angle of the lower lumbar joints
-
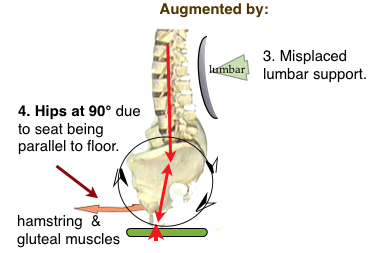
4. Posterior elements
- Stretching of the posterior elements (including ligaments) which can become permanent and allow instability. (☛Ligaments & CTD→) & (see ☛ ‘Liagament integrity & creep’)→
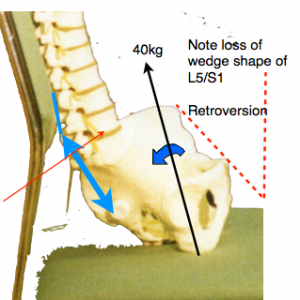 The likely forces that must be resisted by the ilio-lumbar and the supraspinous ligament (shown in blue) when sitting in the usual lumbar support seat, which allows backward tilting of the pelvis, with a bodyweight 40kg (excluding the legs) can be calculated. Simple moments about the centre of the L5 disk suggests a ligament tension of about 70 kg (700 Newtons). This is probably a worst-case estimate. (JD Gorman)
The likely forces that must be resisted by the ilio-lumbar and the supraspinous ligament (shown in blue) when sitting in the usual lumbar support seat, which allows backward tilting of the pelvis, with a bodyweight 40kg (excluding the legs) can be calculated. Simple moments about the centre of the L5 disk suggests a ligament tension of about 70 kg (700 Newtons). This is probably a worst-case estimate. (JD Gorman)
5. Constrained upright sitting
The adverse effects have been long and variously described Prolonged constrained static postures are uncomfortable and deleterious for both spinal and general health. ☛Importance of MOVEMENT→. Recently there has been interest in continuous small amplitude movement for upright chairs, the chair re-aligning with the users centre of gravity, and termed ‘Dynamic Seating’. Exercise is required to maintain this position. This provides proprioceptive feedback and frequent small amplitude pressure changes which may be comforting for short periods and helps multifidus muscle action. Rani Lueder gives a review account (Lueder R 2002) and the referenced evidence→is considerable.
Recapitulation :-
 For the scientific research details, see ☛ bio-mechanics→
For the scientific research details, see ☛ bio-mechanics→
 See ☛ Remediation→
See ☛ Remediation→
The mid-upright mode is the worst possible position. How did it happen? ☛ Why? Mandal explains→
Advocates a Forward Tilted Seat (FTS). The FORWARD TILTED SEAT (FTS).
The upright seat is still recommended….Some of these diagrams suggest that iliac back support is incorporated. This is a partial solution providing it is correctly configured. See ☛ Lumbar support→
The pMRI evidence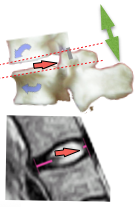
An investigation using Whole-body Positional MRI (pMRI), by FW. Smith, Bashir W (2007) who found that the upright position, at 90°, caused disc contents to move the most, while the relaxed position (135°/45° reclined) caused disc contents to move the least. This confirms that the upright position is the worst for the back, while the relaxed position is the best. See Positional MRI →